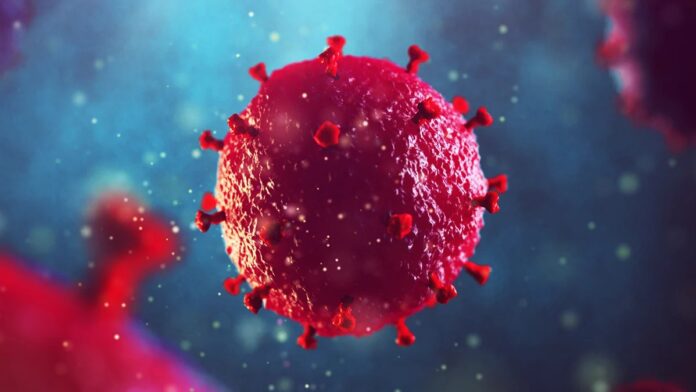
A 63-year-old Norwegian man, referred to in medical literature as the “Oslo patient,” has achieved a rare and significant milestone: long-term remission from HIV. Following a bone marrow transplant from his brother, the patient has maintained a virus-free status for five years without the need for daily antiretroviral medication.
While this case provides a vital roadmap for scientists, it highlights both the incredible potential of genetic research and the extreme medical risks involved in such procedures.
The Mechanism of Resistance: The CCR5 Mutation
The key to this success lies in a specific genetic quirk. During the patient’s treatment for a rare blood cancer, researchers discovered that his brother possessed a rare mutation known as CCR5Δ32/Δ32.
To understand why this matters, one must look at how HIV operates:
– HIV typically enters human immune cells by latching onto a specific receptor called CCR5.
– The Δ32 mutation effectively “deletes” these receptors from white blood cells.
– Without this entry point, the virus cannot penetrate the cells, making the immune system functionally impervious to HIV.
By receiving a stem cell transplant from his brother, the Oslo patient replaced his own susceptible immune system with one that is genetically shielded from the virus.
Why This Case is Scientifically Significant
While several “functional cures” have been documented in medical history, the Oslo patient’s case offers unique data points that distinguish it from others:
1. Clearing the “Viral Reservoir”
The greatest challenge in curing HIV is the virus’s ability to hide in “reservoirs”—dormant pockets of DNA within the body that medication cannot reach. Most cases of remission struggle with the fact that the virus persists in the gut. However, extensive testing on the Oslo patient showed that functioning HIV DNA was cleared even from the gut, which is where the virus most commonly lurks.
2. The Fading Biological Memory
Researchers observed a striking phenomenon: as the virus disappeared, the patient’s immune system stopped reacting to it. HIV-specific T cells declined, and antibody levels dropped. This suggests that once the virus is truly eradicated, the body’s “memory” of the infection also fades, a finding that helps scientists understand the long-term biological markers of a successful cure.
3. The Role of Immune Reactions
The patient experienced graft-versus-host disease (GVHD), a condition where the donor cells attack the recipient’s body. Interestingly, researchers believe this intense immune reaction, along with the drugs used to treat it, may have played a role in helping to “wipe out” the remaining traces of the virus.
The Reality Check: A Cure vs. A Treatment
It is crucial to distinguish between a scientific breakthrough and a practical medical solution.
A bone marrow transplant is not a viable path to a widespread HIV cure for several reasons:
– High Risk: These transplants are “immune system reboots” that carry a mortality rate of 10–20% within the first year.
– Complexity: They are high-intensity procedures reserved for life-threatening blood cancers, not for managing chronic viral infections.
– Specificity: A cure via this method requires a donor with a very specific, rare genetic mutation.
Looking Ahead
The goal for the scientific community is not to perform more transplants, but to extract the “blueprints” from these rare cases. By analyzing the biomarkers and molecular mechanisms present in the Oslo patient and others like him, researchers hope to develop safer, more accessible therapies—such as gene editing—that can mimic this natural resistance without the need for high-risk surgery.
Conclusion
The Oslo patient provides a rare glimpse into what a functional HIV cure looks like at a cellular level. While the transplant method itself is too dangerous for general use, the genetic insights gained from this case are essential for developing future, safer treatments that aim to eliminate the virus’s ability to hide and rebound.